Autoclave or steam sterilization is a moist heat sterilizing technique that has prominent applicability in laboratories, industries, and hospitals to purify different samples, equipment and glassware. It uses high-pressure steam to destroy bacterial cells and fungal spores.
It is one of the types of steam sterilizers that removes contaminants from the goods as a regular pressure cooker does. Here, we will discuss the criteria to maintain the sterility of products through successive stages of the sterilization cycle.
This post describes the meaning, principle, parameters and discoveries that led to the introduction of autoclave sterilization. You will also get to know the basic components of an autoclave, along with the theory of autoclaving, advantages and disadvantages.
Content: Autoclave Sterilization
Autoclave Meaning
An autoclave is a sterilizing machine that makes the equipment and supplies contaminant-free by maintaining pressurized saturated steam under controlled temperature for desired time. The steam pressure and temperature can change depending on the size of loads and contents.
Among chemical, radiation, and gas sterilization methods, a physical means of moist heat sterilization has extensive applicability and the most dependable method. An autoclave is a physical medium of sterilization and disinfection that kills deleterious microorganisms, including bacteria, viruses, fungi etc., on the loads inside a pressure vessel.
History
In the history of autoclave technology, many scientists have contributed that we will discuss below:
- 1681: Denis Papin first invented the pressure cooker that works quite similar to an autoclave. He called this machine a “Steam digester”.
- 1879: A scientist named Charles Chamberland re-invented and devised a machine called an autoclave.
After that, significant advancements in autoclave were made like on control system, autoclave safety, and sterilization cycle.
- 1881: Robert Koch studied the disinfecting properties of steam in concern to an autoclave machine. He concluded that the moist heat (steam) could penetrate more quickly than the dry heat.
- 1933: Modern autoclave machine was introduced with a thermostatic trap and air elimination outlet to maintain appropriate temperature and pressure inside the pressure vessel.
- 1958: Pre-vacuum autoclave technology has been introduced.
- 1987: Modern autoclaves equipped with steam-flush and pressure-pulse were introduced that are recently used in hospitals.
Autoclave Principle
It depends upon the principle of moist heat sterilization, in which goods are exposed to direct steam under controlled temperature and pressure for a specific time. Thus, autoclaving depends on steam quality, pressure, temperature, and time duration. The autoclave uses moist heat, which kills microbial cells, intracellular structures and spores via absolute denaturation. Moist heat coagulates enzymes and structural proteins.
Video: Autoclave Sterilization
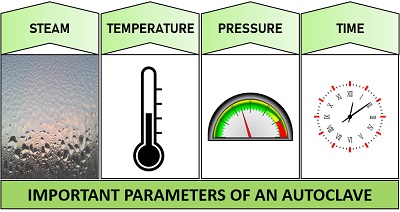
Important Parameters of an Autoclave
The operation and maintenance of an autoclave depends upon the following parameters:
Autoclave Temperature and Pressure
Autoclave uses dry saturated steam under elevated pressure and temperature to ensure potent microbicidal activity. 121°C (250°F) and 132°C (270°F) are the ordinary temperatures maintained in a gravity displacement autoclave and pre-vacuum sterilizer at a standard pressure of 15 and 27 p.s.i, respectively.
The p.s.i (pounds per square inch) is a unit of pressure. If the pressure inside an autoclave is increased above the atmospheric pressure, it will consecutively increase the boiling temperature of the water inside the pressure vessel.
The increase in boiling temperature will turn water into steam by one of its properties, i.e. latent heat of evaporation (heat necessary to turn water into steam or vapours). As a result, the steam penetration into objects placed inside the autoclave increases. Latent heat of evaporation also enhances the killing ability of microbes.
Steam
Quality steam is essential for successful sterilization. The vapour must contain a fraction of 97% steam (vapour) and 3% moisture (liquid water). The steam and moisture ratio is necessary for efficient heat transfer.
For efficient heat transfer, the fraction of steam and moisture must be more than 3%. A fraction less than 3% is considered superheated or dry steam (ineffective for steam sterilization).
Thus, moist heat or heat saturated steam is considered the most effective sterilizing agent to disinfect glassware, culture media, surgical dressings, etc.
Time
The minimal time required to sterilize the contents in the gravity displacement autoclave and pre-vacuum autoclave takes 30 minutes and 4 minutes, respectively, to destroy microbial cells.
The sterilization time may vary depending on the type and load of the contents inside an inner chamber. The heavyweight of glassware, large liquid volumes, and dense materials may increase the sterilization time.
It is recommended that one must operate an autoclave, preferably at high temperatures and short sterilization time over the combination of lower temperatures and longer sterilization time.
Autoclave Basic Components
An autoclave efficiently destroys structural proteins, enzymes, and spores of microorganisms. Generally, there are two kinds of autoclaves, one is gravity displacement, and the other is a pre-vacuum sterilizer.
The working of both differs slightly. The gravity displacement type displaces air through a steam-activated exhaust valve, while pre-vacuum autoclaves drain out the air via the pulling action of the vacuum pump.
Both the models replace air with pressurized steam at the desired temperature and time to maintain a sterile environment inside. In this context, we will look into the basic components of the gravity displacement autoclave. The diagram of an autoclave illustrates the simplicity of operation.
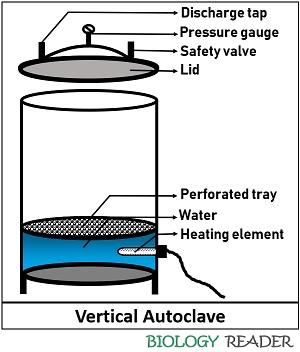
Pressure Chamber
It is the main body that comprises an inner chamber and an outer jacket. An inner chamber is composed of stainless steel. It consists of a tripod stand over which you need to place a perforated holding tray. You can keep the media and glasswares over the holding plate.
An outer jacket used in medical setups is generally filled with steam entering and passing through an operating valve. It flows forward and down through the chamber and reduces the time taken to reach the sterilization temperature. The capacity or size of the pressure vessels ranges from 100 L to 3000 L.
Lid
It is the second most crucial component of an autoclave provided with the following systems:
- Pressure valve: It regulates the pressure of the steam jacket and inner chamber.
- Safety valve: It protects against damages due to overpressure.
- Exhaust valve: It releases steam.
- Whistle: It indicates that the pressure increased inside the vessel by lifting itself to release water vapours.
- Tightening knobs: There are some tightening knobs to lock the autoclave, which form a closed system to sterilize the goods.
Steam Generator
Add water into the inner chamber up to the level of the tripod stand. A power cable is attached to the heating rod necessary for steam production. A heating element or boiler at the bottom of the pressure vessel uses a power supply to generate steam from the water.
The level of water is an essential factor that determines steam sterilizer efficiency. There might get some chances of burning the heating element if the amount of water is too little. Similarly, more than enough water might damage the components placed inside.
Autoclaving
The autoclave has extensive use in practical labs, industries and healthcare settings to sterilize different equipment and media. Items are either wrapped or put directly over the holding plate inside an autoclave chamber under controlled conditions of temperature, pressure and steam upto a specific time.
The working of an autoclave is generally like a pressure cooker, which we use in our daily life to boil or cook food. We could tighten up an autoclave’s door or lid to form a sealed chamber like a pressure cooker. Then, the air displacement systems like steam, steam flushes and vacuum systems remove the air within the pressure vessel, depending upon the type of autoclave.
After that, the pressure within the autoclave facilitates successful sterilization at the desired time by increasing the autoclave’s temperature and killing ability. Later, exhaust the steam after the sterilization of the equipment and media. Therefore, depending upon the working of an autoclave, there are three phases in the autoclave sterilization cycle:
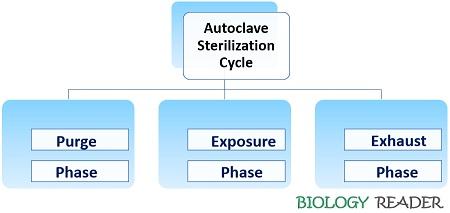
Purge Phase
It also refers to the conditioning phase that involves displacement or removal of the air inside the pressure vessel that may inhibit the sterilization process. Different autoclaves use different methods to remove the air out of the chamber.
- Gravity displacement type autoclave: It uses steam to displace the air.
- Positive pressure displacement type autoclave: It uses steam flushes and pressure pulses.
- Negative pressure (vacuum) displacement type: It employs a vacuum pump to remove all the air.
Exposure Phase
It also refers to the sterilization phase when we need to close the autoclave’s exhaust valve to supply continuous steam into the pressure vessel through a heating element. It causes a rapid increase in the temperature and pressure to the desired setpoint.
Then, items inside the chamber meet the exposure phase under the exposure of sterilization temperature for the desired time depending upon the type and load of content.
Exhaust Phase
The final phase involves the opening of an exhaust valve to release steam out of the chamber or depressurize the chamber. As the steam completely evaporates, take out the items.
Advantages
- Moist heat sterilization is a nontoxic and inexpensive method to conduct.
- Autoclave sterilizer provides a rapid microbicidal and sporicidal effect through its steam saturated with heat.
- Moist heat can penetrate fabrics more effectively instead of dry heat.
- Autoclave sterilizers maintain overall sterility in food and industrial sites by sterilizing the contents required for research purposes.
- Besides, it sterilizes the medical equipment.
- In chemical industries, it helps in hardening the rubber and hydrothermal method.
Limitations
- Moist heat sterilization might cause corrosion and combustion of lubricants.
- Some plasticware might melt under high heat.
- Many chemicals break down during the sterilization process.
- The heat produced in autoclaves takes much more time to sterilize solid media and large containers.
Conclusion
Therefore, we can conclude that autoclave sterilization is the best way to sterilize culture media, pipette tips, equipment and glassware. It is also useful to inactivate the bacteria, viruses, fungi, and yeasts in culture plates, medical and surgical wastes via autoclaving prior to disposal.
Is it necessary to do a liquid sterilization prior to autoclaving?