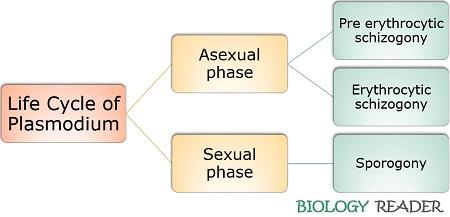
The life cycle of Plasmodium species generally exist within two phases (asexual and sexual) or require two living hosts (vertebrates and mosquito). Plasmodium’s asexual phase begins within the female Anopheles mosquito’s stomach, while the sexual phase starts within the human beings’ hepatic cells. Thus, the life cycle of Plasmodium mainly involves two hosts, namely a primary host (man) and a secondary host (female Anopheles mosquito).
Systemic Classification:
- Phylum: Protozoa
- Sub-phylum: Plasmodroma
- Class: Sporozoa
- Order: Telosporodia
- Genus: Plasmodium
Its sexual phase is anisogamous, and the asexual phase occurs through binary fission. Here, you will get to know the elaborative study of the asexual and sexual stages in the Plasmodium’s life cycle.
Content: Life Cycle of Plasmodium Species
- What is Plasmodium?
- Asexual Lifecycle of Plasmodium
- Sexual Lifecycle of Plasmodium
- Video
- Summary
- Conclusion
What is Plasmodium?
Plasmodium is a malaria parasite that generally includes four species, P. vivax, P. ovale, P. falciparum and P. malariae, where all the species cause four distinct types of malaria. They possess a digenetic life cycle. The sexual life cycle of Plasmodium is called sporogony, whereas the asexual life cycle of Plasmodium is called schizogony.
Plasmodium species are endoparasites which infect and reside within the host cells. Plasmodium species lack locomotary organs but move through the bloodstream from one host to the other.
Asexual Lifecycle of Plasmodium
The asexual lifecycle of Plasmodium involves five stages:
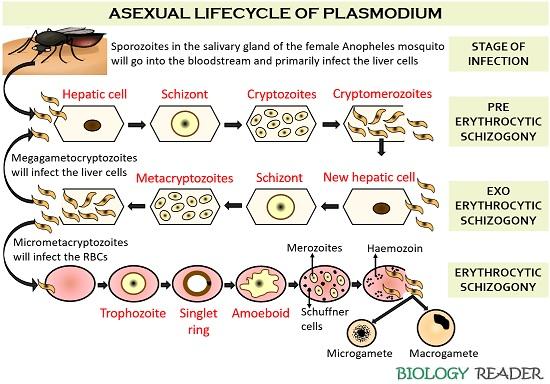
Stage of Infection
It is the stage when the sporozoites enter the bloodstream via a mosquito bite. The sporozoites then find out their way to infect the liver cells.
Pre-erythrocytic Schizogony
This stage can be defined as the infection phase of the liver cells. It involves a series of morphological changes that are discussed below:
- Firstly, the sporozoites released from the female Anopheles mosquito’s salivary gland will penetrate the hepatic cell wall through some lysosomal enzymes.
- Then, the sporozoites harness the liver cells’ essential components to nourish themselves. The sporozoites that attained a large size are called schizonts.
- After that, a schizont will divide to increase its number and form cryptozoites.
- The cryptozoites will again increase their size and number to produce cryptometazoites.
- Eventually, a hepatic cell becomes laden with the numerous cryptometazoites, and it will burst out, resulting in the release of cryptometazoites.
Exoerythrocytic Schizogony
It is a stage before the infection of RBCs. Here, the cryptometazoites released from a liver cell will infect other new liver cells. Exoerythrocytic schizogony involves the following morphological changes.
- The cryptometazoites will again penetrate the wall of new hepatic cells.
- They will then invade the nutrients and other essential components of the hepatic cells to form a schizont.
- Schizonts will divide and grow in number to produce metacryptomerozoites.
- Ultimately, a liver cell laden with a large number of metacryptomerozoites will burst out, and it will release all the infectious particles into the bloodstream.
Erythrocytic Schizogony
It is the stage of RBC infection. In this stage, the metacryptomerozoites or merozoites will infect the erythrocytes. The metacryptomerozoites will penetrate the wall of RBCs through the activity of hydrolytic enzymes. Once the merozoites enter into the RBC, they will start utilizing the content of RBC, i.e. haemoglobin, to form a trophozoite.
A trophozoite goes through various morphological changes, which we can see in the above picture. A signet ring stage occurs, in which a trophozoite increases its size and forms a large non-contractile vacuole. Later, an amoeboid stage replaces the signet ring stage.
The trophozoite wall becomes irregular during an amoeboid stage, resulting in the complete breakdown of haemoglobin content into haematin and globin. Then, the amoeboid stage transforms into erythrocytic schizont, which further undergoes cell division to form merozoites.
We could observe schuffner cells and haemozoin granules (deposits of haematin) during the merozoite stage. A rosette stage appears at the end of the erythrocytic phase, where the merozoites shift towards the RBCs’ periphery. The lysis of RBC occurs at the end of the erythrocytic phase once a cell becomes laden with enough merozoites.
Formation of Gametocytes
The merozoites in the bloodstream will differentiate into two distinct gametocytes, namely macrogametocytes and microgametocytes. Thus, the merozoites will form gametocytes instead of schizonts after several generations of erythrocytic schizogony. The characteristic difference between the macrogametocytes and microgametocytes of Plasmodium is given below in the table.
| Properties | Macrogametocytes of Plasmodium | Microgametocytes of Plasmodium |
|---|---|---|
| Type of gamete | It produces female gametes | It produces male gametes |
| Size | Large in size (10-12 µ) | Comparatively smaller (9-10 µ) |
| Number | These are found less in number | These are found large in number |
| Nucleus | It comprises of a small peripheral nucleus | It comprises of a large central nucleus |
| Reserve food material | Present | Absent |
| Cytoplasm | Dark in colour | Light in colour |
| Motility | Non-motile | Motile |
Macrogametocytes and microgametocytes will remain in the bloodstream of an infected person. Once a female Anopheles sucks the blood of an infected person, the gametocytes will further differentiate in the mid-gut of the mosquito, and there the sexual reproduction of the Plasmodium begins.
Sexual Lifecycle of Plasmodium
It is also called gametogony. During the sexual reproduction of the malaria parasite (Plasmodium), the gametocytes of the infected person’s blood will further differentiate and undergo fertilization to form a zygote in a female Anopheles mosquito’s stomach. Thus, the blood sucked by the Anopheles mosquito will primarily enter the mid-gut and later move towards the salivary gland.
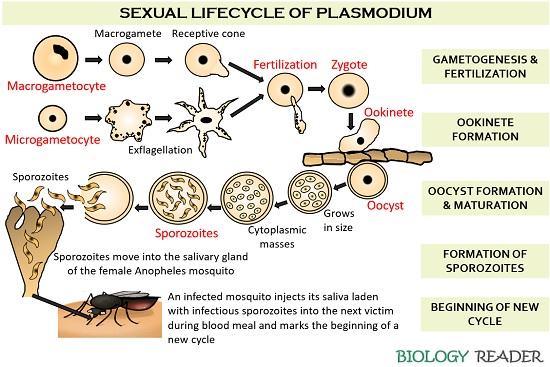
Formation of Gametes
The female gametocytes, i.e. macrogametocytes, go through some morphological changes that form macrogametes that eventually differentiate into receptive cones.
Oppositely, the male gametocytes (microgametocyte) will undergo exflagellation in the mid-gut of the Anopheles mosquito to form 6-8 flagellar-like microgametes. Thus, the motile microgametes will freely move inside the stomach of the Anopheles mosquito in search of macrogametes or female gametes.
Fertilization
Then, the fertilization or the fusion of macro and microgametes will occur, resulting in a spherical zygote formation. After 8-10 hours, a spherical zygote differentiates into an ookinete stage.
Ookinete differentiation into Oocyst
An ookinete reaches the epithelium midgut through its gliding motility and penetrates the peritrophic matrix of the mosquito. As a result, ookinete will encyst into an oocyst on the midgut basal lamina.
Sporogony
After that, numerous sporozoites form after the maturation of the oocyst, followed by nuclear and cytoplasmic divisions. Sporozoites will rupture the oocyst wall, and then it finds their way to enter the mosquito’s salivary gland.
Beginning of a new cycle
Thus, the infectious sporozoites reside in the saliva of the female Anopheles mosquito. When the infected mosquito takes a blood meal, it injects the saliva laden with infectious sporozoites into the next victim by marking a new cycle.
| Phases in the life cycle of Plasmodium | Meaning | P. vivax | P. ovale | P. malariae | P. falciparum |
|---|---|---|---|---|---|
| Pre erythrocytic schizogony | It is the stage where the sporozoites infect the hepatic cells | 6-8 days | 9 days | 14-16 days | 5-7 days |
| Erythrocytic schizogony | It is the stage where the merozoites infect the red blood corpuscles | 48 hours | 50 hours | 72 hours | 48 hours |
| Sporogony | It is the stage where the gametes fuse to form a zygote that goes through a several developmental stages to form sporozoites | 8-10 days | 12-14 days | 14-16 days | 9-10 days |
| Incubation period | It is the time between the stages of infection till the symptoms appear | P. vivax has an incubation period between 12-17 days, and it causes benign tertian malaria | P. ovale causes benign quaterdian malaria with an incubation period of 16-18 days | P. malariae has an incubation period of 28 days, and it causes benign tertian malaria | The most critical type of malaria (malignant tertian malaria) is caused by P. falciparum, and its incubation period is between 14-16 days |
Video: Malaria and Life Cycle of Plasmodium
Summary of Plasmodium’s Life Cycle
Let us take a quick review of the Plasmodium’s life cycle by looking into the process summarized below:
- Mosquito acts as the definitive host of the Plasmodium parasite, which facilitates the injection of the malarial parasite along with its saliva into the blood of an intermediate host (man). Thus, the inoculation of the parasite will result in various clinical manifestations of malaria.

- The initial symptoms include fever, chills, headache, weakness, vomiting and diarrhoea. Sometimes, complications like splenomegaly, anaemia, thrombocytopenia and hypoglycaemia may also occur.
- A few hundred sporozoites from the mosquito’s salivary gland will enter the human body, where the macrophages destroy many of them.
- The remaining sporozoites penetrate the liver cells after travelling through the lymphatic system into the blood vessels. The sporozoites enter the hepatocytes after crossing the wall of the liver sinusoid.
- Inside the hepatic cells’ parasitophorous vacuole, the sporozoites grow and multiply their number to develop schizonts.
- Schizonts further divide to produce numerous merozoites (10-000-30,000 or even more) packaged within the merosome vesicles (protects from the phagocytic Kupffer cells).
- The pre-erythrocytic schizogony lasts 5-16 days and generally imposes little or no symptoms.
- Some sporozoites will stay dormant in the hepatic cells as hypnozoites, while a few will proceed to infect the other cells (particularly RBCs) and initiates erythrocytic schizogony. Within the RBCs, the malarial parasite goes through a repeated cycle of parasitic development.
- The merozoites enter the RBCs through attachment and invasion through components like micronemes, rhoptries and dense granules.
- The merozoites invade haemoglobin for their growth and development by ingesting it into a food vacuole. Then, they degrade the haemoglobin proteins into amino acids and utilize them for the protein synthesis of Plasmodium.
- Heme is a remaining toxic component detoxified by the heme permease and found as the cell deposits in the form of haemozoin granules (Malaria pigment).
- Then, the merozoites transform into gametocytes that are extracellular and non-pathogenic. The gametocytes remain in an infected man’s blood, but their further developmental stages occur within the definitive host (mosquito).
Conclusion
Therefore, a life cycle of Plasmodium repeatedly occurs between the two hosts (mosquito and man). A malarial parasite and mosquito show a mutualistic relationship, in which both the Plasmodium parasite and the mosquitoes are equally benefitted.
According to the study, it was observed that the mosquitoes infected with Plasmodium have better survival and better blood-feeding rate. Similarly, the Plasmodium species get benefitted from the definitive host mosquito that helps them invade the host cell’s nutrients (mainly vertebrates) to increase their population.